The challenges patients face during active cancer treatment are not limited to the clinic or hospital walls. Frequently, they extend into the home, where patients and caregivers are tasked with managing adverse effects (AEs), assessing their seriousness, and seeking medical attention when necessary. For some, this stress is compounded by living alone without a caregiver, forcing patients to make these decisions by themselves.
Advances in oncology—from bispecific antibodies and antibody-drug conjugates to chimeric antigen receptor (CAR) T-cell and radioligand therapies—are transforming patient outcomes but also introducing more complex and evolving toxicity profiles. Traditional care models based on episodic consultations or phone calls offer limited visibility into how patients are doing between visits.
Electronic patient-reported outcomes (ePROs)—a tool allowing patients to record and submit their symptom burden and functional status digitally—can address this blind spot. Yet, many solutions remain generic in their workflows and mainly help capture AEs between visits, but do not help care teams to proactively manage or prevent them from worsening.
Cureety offers a new kind of ePRO solution, specialized in oncology and designed to make care better quality, more efficient, and more proactive for all patients. To learn more about how Cureety can support the entire care team, ACCCBuzz spoke with Misha Kaur, chief operating officer.
Where Traditional Platforms Can Be Limited
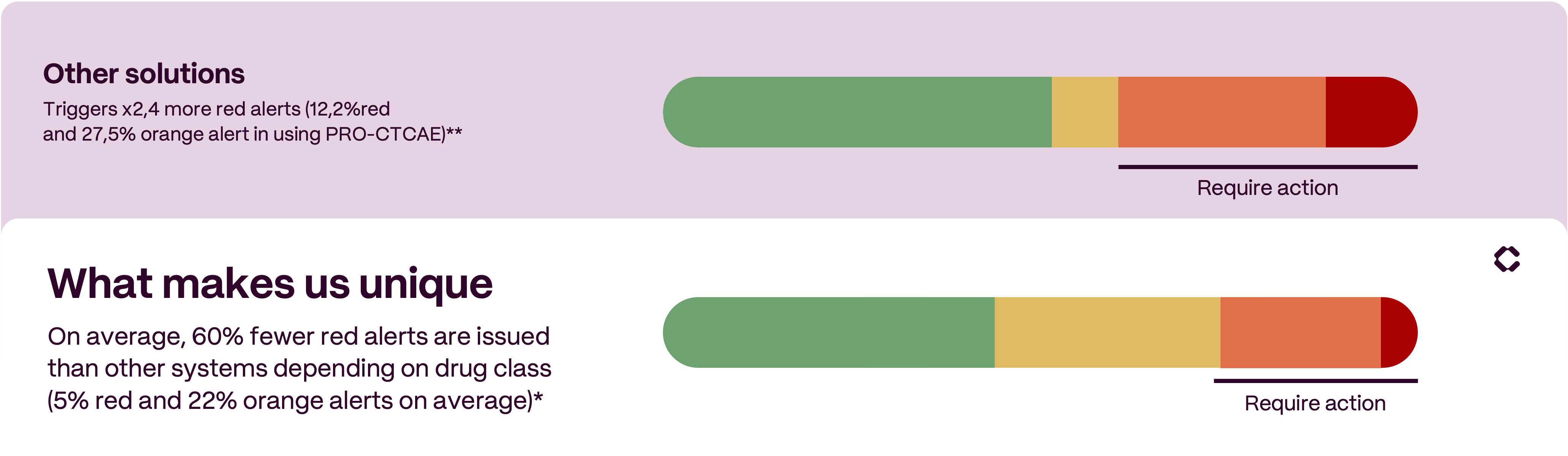
Many remote symptom monitoring solutions rely on generic instruments that struggle to capture the clinical nuances of modern cancer therapies and can risk generating incomplete information or excessive alert noise for care teams. The standard lexicon for AE reporting in oncology is the Common Terminology Criteria for Adverse Events (CTCAE). PRO-CTCAE was later developed as a companion tool, allowing patients to self-report symptomatic toxicity across multiple dimensions such as frequency, severity, and interference.
Many digital symptom monitoring solutions draw on PRO-CTCAE because it provides a comprehensive taxonomy. However, this can have limitations in routine care settings. Depending on how it is applied, patients may be asked to respond to questions that may not be directly relevant to their specific cancer type or therapy, making symptom reporting less precise.
Reducing Patient and Provider Burden
Cureety is committed to supporting patients as soon as they receive a cancer diagnosis and throughout their entire journey—including when they’re at home. “We do that through ensuring our questionnaires use objective patient-centered language and are treatment-specific. This helps providers clearly understand symptom burden, while offering patients educational tools and resources personalized to their responses and context, so they feel empowered to engage with their own care,” said Kaur.
Where Cureety departs from more traditional ePRO platforms is not only in what it asks, but how it asks it. Cureety has a scientific committee–validated CTCAE-aligned questionnaire built around clinically relevant toxicities for each treatment, so patients are only tasked with answering relevant questions.
“This is something we prioritized based on clinician input, patient feedback, and research showing that most solutions use questionnaires that are too subjective or difficult for patients to interpret or respond effectively,” said Kaur. For example, a patient may be asked to use a 5-point scale (none to very severe) to answer What was the severity of your cough at its worst? One patient’s answers would likely differ from the rating of another patient with the same severity of cough, and from how the clinician may interpret it.
Cureety instead frames its questionnaires around objective, patient-friendly language aligned and graded using CTCAE. “For example, if asking about cough, responses would be written as: persistent cough that causes insomnia and may be accompanied by vomiting, and shortness of breath and difficulty breathing. These measures are mapped back to the CTCAE standards for grading, which results in more accurate symptom reports from patients, reduced guesswork, and information that is more closely aligned with clinical grading—while also cutting down the number of questions,” Kaur explained.
This reduced burden is key, as patients are already navigating a difficult and overwhelming period in their lives. Making it easy for them to report the right issues, in the right way, is essential both for engagement and safety.
Clinically Specific Triage Without Alert Fatigue
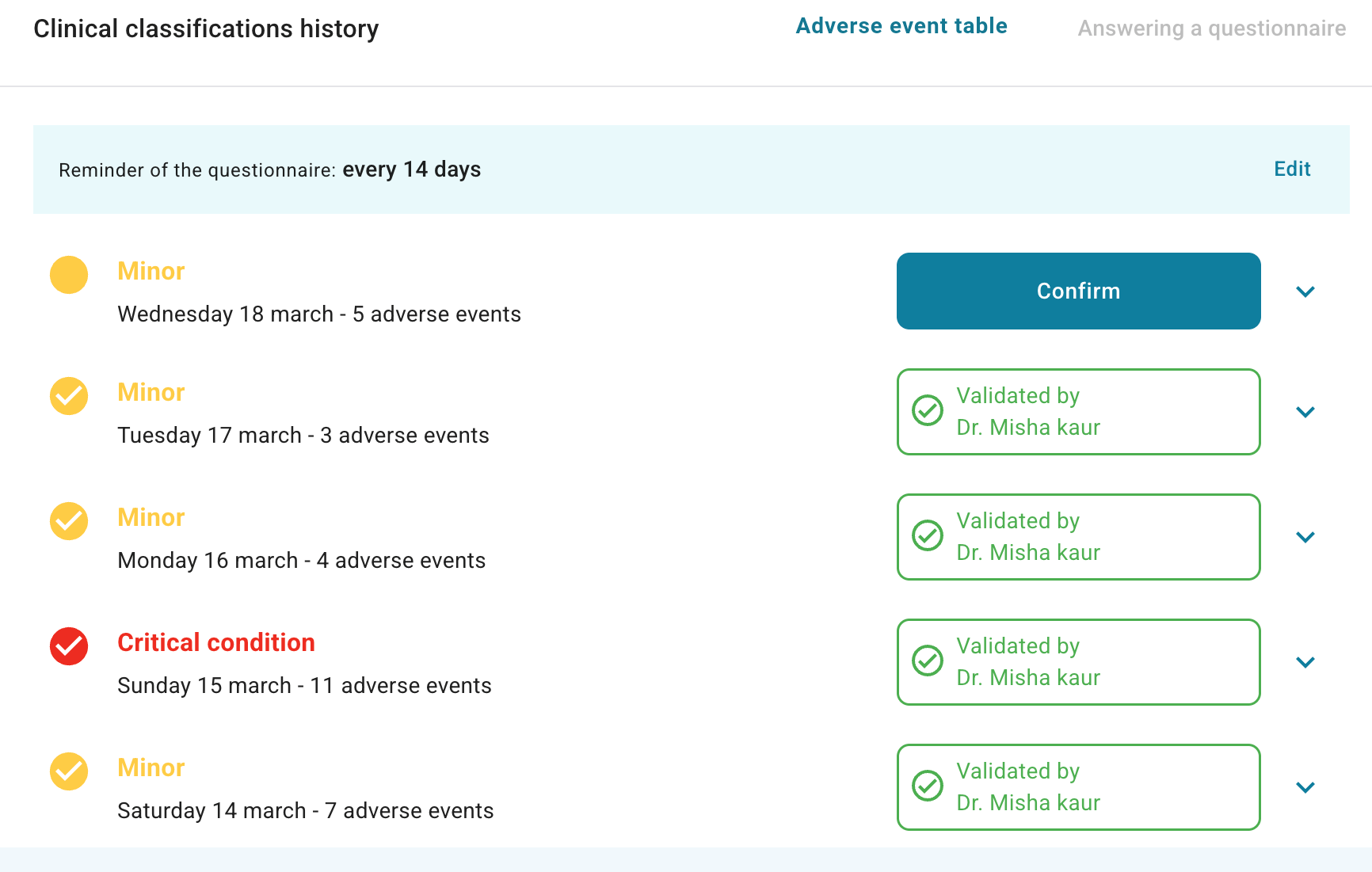
Cureety also differentiates itself in how reported symptoms are classified and translated into alerts for care teams. “In oncology, the same symptom—or even the same severity grading—does not always carry the same clinical significance across therapies. The meaning of a symptom depends heavily on treatment context,” Kaur noted. “This is why Cureety uses a proprietary therapy-specific triage classification system, recognizing that certain symptom combinations require different escalation thresholds, depending on the treatment being administered.”
Take, for example, a patient receiving CAR T-cell therapy, for whom cytokine release syndrome is a major risk. In this context, even a mild fever can represent an early warning sign that requires immediate clinical attention. In more generic monitoring, this type of symptom may not always trigger rapid escalation. Cureety’s triage system is designed to recognize these specific risks and generate alerts at the right time for clinicians.
Furthermore, Cureety’s solution is designed to be highly specific and highly sensitive, generating relatively few red alerts and fewer false positives. “One drawback of many digital monitoring systems is that they can create more work for providers,” said Kaur. “We’re interested in producing robust, trustworthy results that allow clinicians to actively monitor their patients safely without having to do it manually, knowing that they will receive an alert to help them prioritize which patients need a consult earlier, when it matters most.”
A Use Case in Functionality, Impact, and Reassurance
A participant in one Cureety case study discussed the change before and after implementing Cureety’s solution. Prior, it was difficult for her team to stay connected to patients between hospital visits for a variety of reasons: consultation times are limited, and many patients don’t report all relevant AEs because they don’t know exactly what to look for. Then they would go home, feel anxious about a symptom, and try to call the hospital, resulting in a lot of manual call fielding.
“They needed a continuous thread of care that extends beyond the clinic walls,” said Kaur. “Our platform offered visibility of their patients, providing them with important real-time information that enabled them to take action quickly.” Blind spots are a key challenge in cancer care; Cureety’s platform has demonstrated a 61% reduction in toxicity-related hospitalization duration.
The platform also offers a mechanism for patients to indicate if they have a specific concern or additional information, opening up a communication channel to their care team that is centralized and easy to use, rather than calling in. Cureety reduces unnecessary manual administration so providers can concentrate on what matters most. Another case study yielded a 43% decrease in the number of calls for clinicians.
Another challenge with digital health solutions is patient adherence. To address this, feedback mechanisms are built into Cureety, so patients feel connected and see the value of engaging with Cureety. “This gave patients a strong sense of reassurance and improved treatment adherence. It shows them that even if they’re far away, another human being has engaged with their response,” said Kaur.
“More and more people are living longer with cancer, many of them living alone without caregivers. This, coupled with more therapies moving to outpatient or community delivery settings means it is so important to make them feel connected to their care team no matter who or where they are,” Kaur emphasized.
Growth Across Borders With the US as a Key Priority
Cureety has supported more than 60,000 patients through their treatment journeys. Though born in France—and now partnered with over 50% of comprehensive cancer centers in the nation—Cureety is rapidly growing internationally, with a presence in Portugal and Italy, and growth in Belgium, Germany, and the United States in 2026.
“We consider growth in a few ways: value and mission, product adaptation, and localization,” Kaur explained. Her team is exploring partnerships and establishing reference sites as pilots as they adapt their product to the unique workflows of the US health system. “Solutions like this are best when they are built with care teams. When we integrate with the system and its workflows, we know the value is optimized, so we take a lot of time to ensure the product is fit for the context. We work closely with health care providers during implementation and to support the embedding of the solution into workflows.”
As Cureety expands, Kaur’s team is collaborating with a diverse array of oncology practices in the US. “We’re committed not just to finding long-term partners for pilot collaborations, but also facilitating robust studies to demonstrate the impact of our solution in the US and to support our broader strategy to achieve reimbursement around the use of remote therapeutic monitoring in oncology,” said Kaur. Her team is also seeking physicians, clinicians, and navigators to act as an advisory board.
The Next Generation of Cancer Care
“Remote monitoring works best when it’s designed with both clinical robustness and human connection in mind,” Kaur emphasized. “In my mind, the next generation of cancer care will be deliberately designed to leverage both digital and human elements to be greater than the sum of its parts, because we are not trying to replace relationships. It’s about preserving them—enabling care teams to be more present, more proactive, and more human to support patient-centered, quality care.”
For more information about Cureety and how your cancer program or practice can collaborate, contact Misha Kaur at misha.kaur@cureety.com.
Resources