Sustaining care delivery during the COVID-19 pandemic has required cancer programs and practices nationwide to quickly adopt and expand telehealth services. The Centers for Medicare and Medicaid Services (CMS), private payers, and state regulatory bodies have helped enable a remarkably rapid expansion of telehealth by removing the reimbursement and legislative barriers that had long impeded broad telehealth adoption. The result was immediate: Approximately 1.3 million Medicare beneficiaries received telehealth services in the week ending April 18, compared to 11,000 in the week ending March 7, representing an increase of more than 11,718% in just one and a half months.
As uncertainty continues amid the COVID-19 public health emergency, providers and patients are embracing telehealth to meet specific care needs. Cancer practices and programs are honing its use, demonstrating how telemedicine can enable new approaches to expanding access to care to traditionally underserved groups and under-resourced suburban and rural areas.
Many providers and payers are lobbying for the waivers that have enabled the current widespread use of telehealth to become permanent, and there are signs that might happen. Seema Verma, CMS administrator, has said in reference to telehealth’s explosive growth, “I can’t imagine going back.”
This educational initiative addresses the immediate and ongoing needs of cancer programs and practices that want to implement, integrate, and expand their telehealth services to optimize patient care and aims to educate the multidisciplinary cancer team on how to optimize telehealth by providing resources and information to keep telehealth an essential component of quality cancer care.
For more information on this project, please contact the ACCC Provider Education department.
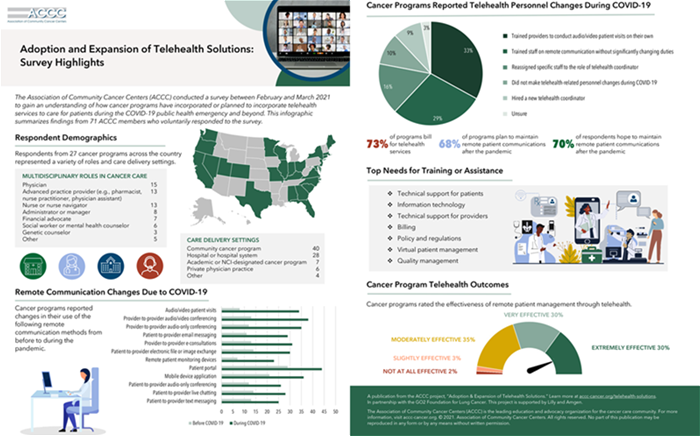
Survey Highlights
A survey was conducted between February and March 2021 to gain an understanding of how cancer programs have incorporated or planned to incorporate telehealth services to care for patients during the COVID-19 public health emergency and beyond. This infographic summarizes findings from 71 ACCC members who voluntarily responded to the survey.
Telehealth in Action
ACCC documented successes in the cancer care community’s rapid adoption of telehealth to maintain patient care during the COVID-19 public health emergency. To obtain multiple perspectives on best practices in team-based telehealth delivery, ACCC conducted multidisciplinary focus groups with the following member sites:
- Cone Health Cancer Center
- Winship Cancer Institute of Emory University
- Texas Oncology
ACCC also conducted interviews with oncology professionals across the country—including a financial advocate, an information technology (IT) professional, a nurse, an oncologist, a pharmacist, and social workers—to learn how their roles were impacted by—and adapted to—the growing need for telehealth services since the onset of the pandemic.