Re-structuring care delivery to be more patient centered is among the many demands the U.S. healthcare system is striving to meet. The imperative to center care around engaged patients is recognized by regulators, health systems, hospitals, professional societies, providers, payers, and patients and families—and it is a central component of value-based care.
Of the Institute for Healthcare Improvement Triple Aim domains to achieve optimal health system performance, the first is: Improve the patient experience of care (including quality and satisfaction).
At last week’s 35th ACCC National Oncology Conference in Phoenix, featured speaker Julie Oehlert, DNP, RN, took issue with patient “satisfaction” as a metric for the patient experience. Healthcare “has gone down the customer satisfaction route as a measure of quality,” she said, “. . . can patients [ever] be ‘satisfied’ with a diagnosis of cancer?” Even though many healthcare organizations have moved from “patient satisfaction” to the concept of patient experience, “We didn’t move our strategies or tactics to measure this. We used the same old customer service tools.”
To move the needle on patient experience, she believes we must start by recognizing that “healthcare is a relationship between those who provide care and those who seek care.”
Recalling an article by Thomas Bodenheimer, MD, and Christine Sinsky, MD, (Annals of Family Medicine, 2014) that makes the case for moving from the Triple Aim to the Quadruple Aim, with the addition of “improving the work life of health care clinicians and staff,” Oehlert concurs. “You won’t hit the IHI Triple Aim unless you add the Quadruple Aim of improving health and well-being of staff.”
Today, the issues of burnout and the well-being of clinicians and healthcare team members are a national concern. In 2017 the National Academy of Medicine established its Action Collaborative on Clinician Well-Being and Resilience. The Collaborative's website outlines multiple factors contributing to the problems of burnout and stress, acknowledging that “Organizational leadership, culture, and policies can play a significant role in burnout and well-being.”
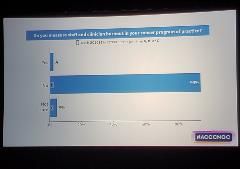
Yet in a pop-up poll during Dr. Oehlert’s presentation, 93% of conference attendees said that their cancer program or practice did not measure staff or clinician burnout.
This scenario is something Dr. Oehlert hopes to see turn around. At Vidant Health, the “journey to promote a caring and compassionate culture,” is already underway. At the health system, she is responsible not only for the patients’ experience but also for the team members’ experience. The focus is on the “BIG E—Everyone’s Experience Matters,” she said. “How we [the healthcare team] experience each other begets the patient experience.”
___________________________________________________
ACCC President Tom Gallo’s presidential theme is “Reflect, Renew, Reignite: Building a Resilient Oncology Team in Your Community.” How is your cancer program addressing team well-being and fostering resilience? If your cancer program has a wellness initiative underway, contact us. Be sure to visit the NAM Action Collaborative Knowledge Hub for resources and tools.