The Froedtert & Medical College of Wisconsin (MCW) Blood and Marrow Transplant and Cellular Therapy (BMT) Program at the health network’s Froedtert Hospital campus has a long-standing history of excellence in cancer care and blood and marrow transplantation research. Since performing its first autologous stem cell transplant in 1982, the program has grown significantly, now conducting more than 350 transplants annually.
In 2009, the BMT Program expanded its offerings by introducing autologous transplants as an outpatient service. This shift aimed to enhance patient access, comfort, and convenience while achieving institutional cost savings. Following this success, the program soon extended to allogenic transplants. More recently, the emergence of immunotherapies such as chimeric antigen receptor (CAR) T-cell therapy has transformed the landscape of cancer care across multiple disease types. Administration of CAR T-cell therapy initially required hospital admission, but it has since been identified as a viable option for select patients to receive on an outpatient basis. With available commercial CAR T-cell products, as well as CAR T-cell products manufactured in an onsite cellular therapy lab, the Froedtert & MCW health network was confident it could safely offer CAR T-cell therapies in the outpatient setting. The goal was to maximize patient access and convenience and to uphold the health network’s commitment to value-based care.
Program Inception and Goals
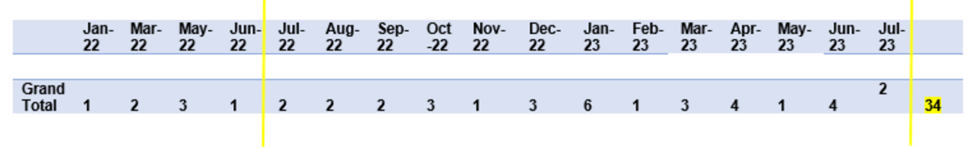
Development of the outpatient CAR T-cell therapy program began in early 2021, culminating in the administration of the first FDA-approved outpatient CAR T-cell product in January 2022. Prior to this milestone, all CAR T-cell therapies, whether clinical or research-based, required inpatient admission at Froedtert Hospital. Since the program’s inception, an increasing number of patients have successfully received CAR T-cell therapy on an outpatient basis, including complete lymphodepletion, CAR T-cell infusion, and management of mild cytokine release syndrome (CRS) (see Table 1).
Table 1: Volume of PatientsReceiving CAR T-Cell Therapy in an Outpatient Setting (January 2022 – July2023)
Literature Review
During the year-long preparation and development of the outpatient CAR T-cell therapy program, several key publications and educational materials provided invaluable guidance. Kristin Kingma, a key figure in the program’s development, highlighted several of these resources as particularly instructive. The most pertinent findings from these publications are summarized in Table 2, offering crucial insights for any cancer center looking to operationalize a similar program.
Topic
Source
Key Findings and Program Takeaways
Program development
Borogovac A, Keruakous A, Bycko M, et al. Safety and feasibility of outpatient chimeric antigen receptor (CAR) T-cell therapy: experience from a tertiary care center. Bone Marrow Transplant. 2022;57(6):1025-1027. doi:10.1038/s41409-022-01664-z
The sequential steps necessary to develop an outpatient CAR T-cell therapy program include:
- ·Create a multidisciplinary team.
- ·Train clinically competent nursing staff.
- ·Alert and educate providers in the community.
- ·Augment patient knowledge and support.
- ·Acquire physical space.
- ·Continuously review outcomes and procedures.
Treatment course
Majzner RG, Mackall CL. Clinical lessons learned from the first leg of the CAR T cell journey. Nat Med. 2019;25(9):1341-1355. doi:10.1038/s41591-019-0564-6
Schmidts A, Wehrli M, Maus MV. Toward better understanding and management of CAR T -cellassociated toxicity. Annu Rev Med. 2021;72:365-382. doi:10.1146/annurev-med-061119-015600
CAR T-cell therapy offered in the outpatient setting involves the same course of treatment as is given while treating patients in the hospital (ie, evaluation, conditioning, infusion, engraftment, and recovery).
Patients at high risk for CRS toxicity or other complications are not candidates for outpatient CAR T-cell therapy. They may, however, be eligible to receive lymphodepletion on an outpatient basis.
Known barriers to keep in mind and continuously evaluate:
- ·Prevalence and incidence of CRS.
- ·Patient status is dynamic, regardless of setting.
- ·Manufacturers of investigational CAR T-cell products usually require inpatient administration and care delivery.
Outpatient criteria
Brudno JN, Kochenderfer JN. Recent advances in CAR T-cell toxicity: mechanisms, manifestations and management. Blood Rev. 2019;34:45-55. doi:10.1016/j.blre.2018.11.002
Lee DW, Santomasso BD, Locke FL, et al. ASTCT consensus grading for cytokine release syndrome and neurologic toxicity associated with immune effector cells. Biol Blood Marrow Transplant. 2019;25(4):625-638. doi:10.1016/j.bbmt.2018.12.758
Assessment
- ·A full evaluation is required todetermine the appropriateness and safety of outpatient treatment.
- ·The patient must otherwise be in good physical condition with no significant comorbid medical problems (eg, heart or kidney disease).
Accessibility
- ·Patients should live within 45 min to 1 hour from hospital.
- ·They should be willing to stay at a designated hotel or lodging for the duration of treatment.
Accountability
- ·The patient should have a responsible caregiver(s) who is available to accompany them to all appointments and provide 24/7 care, support, and transportation during treatment.
- ·The patient must be able to make daily visits to the outpatient setting.
Admission criteria
Brudno JN, Kochenderfer JN. Recent advances in CAR T-cell toxicity: mechanisms, manifestations and management. Blood Rev. 2019;34:45-55. doi:10.1016/j.blre.2018.11.002
Lee DW, Santomasso BD, Locke FL, et al. ASTCT consensus grading for cytokine release syndrome and neurologic toxicity associated with immune effector cells. Biol Blood Marrow Transplant. 2019;25(4):625-638. doi:10.1016/j.bbmt.2018.12.758
The criteria for hospital admission (adopted from literature) are as follows:
- ·Altered mental status (AMS) or any neurological changes consistent with immune effector cell-associated neurotoxicity syndrome (ICANS)
- ·Fever >100.4oF in a neutropenic patient (ANC <500)
- ·Hypoxia (SpO2 <91%) with or without severe dyspnea
- ·Persistent hypotension after fluid resuscitation
- ·Suspicion of an acute infectious process requiring intravenous medical management
Table 2: Key Publicationsand Summary of Evidence-Based Findings on Implementing an Outpatient CAR T-CellTherapy Program
Program Operationalization
As the outpatient CAR T-cell therapy program was rolled out, several logistical considerations emerged as critical. It was deemed necessary that to be eligible for outpatient treatment, patients were required to reside within 45 minutes of Froedtert Hospital or secure nearby accommodation during their treatment. Collaboration with community nonprofit organizations, such as Kathy’s House, played a crucial role in this regard. Kathy’s House offers discounted lodging rates for outpatient program patients, with amenities including private rooms, baths, kitchens, and shared community spaces. Additionally, oncology social workers facilitated connections with local Airbnb options as needed.
From an operational standpoint, Kristin Kingma, clinical nurse specialist at Frodtert & MCW, emphasizes the importance of having a dedicated quality and compliance professional to oversee necessary details, such as environmental concerns that may otherwise be overlooked (eg, maintaining accurate building thermostat logs). In addition, the Froedtert & MCW 24-hour Cancer Clinic was essential for the program’s success, ensuring that patients had access to a higher level of care as needed. Regular debriefing sessions strengthened the relationship with the 24-hour Cancer Clinic, refining the process for making timely admission decisions. Notably, nearly all patients in the BMT Program presented with fever, requiring workups for infection and interventions with medications such as tocilizumab, intravenous fluids, and imaging.
Conclusion
After more than a year of full operation, the outpatient CAR T-cell therapy program has demonstrated significant impact through various outcome measures. Although a considerable proportion of patients (up to 75%) required admission at some point, the program succeeded in saving around 432 bed-days overall. These results underscore the program’s success in enhancing patient care while also contributing to the institution’s financial sustainability. Eager to share the outpatient CAR T-cell therapy program’s success, Kristin Kingma is happy to elaborate on details of the Froedtert & MCW program with other organizations looking to implement similar efforts. She can be reached at: kristin.kingma@froedtert.com.
Resources
OncologyPractice Transformation and Integration Center (OPTIC)
BringingCAR T-Cell Therapies to Community Oncology
Tipsfor Early Patient Identification for CAR T-Cell Therapy and Care Continuitywith Community Providers